Authored by Associate Professor Vicki Kotsirilos AM,
MBBS, Hon Fellow RACGP, FACNEM, FASLM
Associate Professor Vicki Kotsirilos AM is a GP in Melbourne. She is an adjunct associate professor at the University of Western Sydney.
15 August 2021
The COVID-19 pandemic has impacted the whole world and the way that we all live!
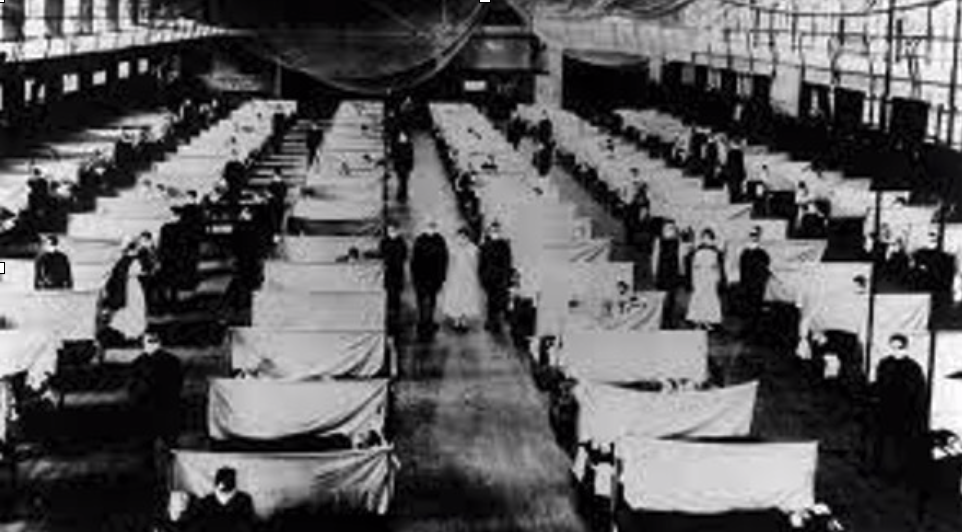
Influenza pandemic Jan 1918 to Dec 1920
We have experienced pandemics before. For example, soldiers fighting at the end of World War I spread the Influenza virus around the globe. In October 1918, San Francisco went through a second wave and the hospitals suffered a rapid rise in the number of infected patients. About a 1/3rd of the world's population, i.e. about 500 million people were infected by the influenza virus leading to an estimate of about 50 million deaths at the time. Current worldwide cases from COVID-19 infection at the time of writing this article [14th September 21] is around 226M cases and to date has caused about 4.65M COVID related deaths. Wearing facial masks in public became mandatory in the United States for the first time and mask-wearing laws largely had public support.

Doherty Institute modelling studies
The Doherty Institute modelling studies suggest Public Health measures such as wearing facial masks, physical distancing and short lockdowns when required will continue to play an important role even with widespread population vaccination. It is likely COVID will be around for some time! So, developing resilience with ongoing needs to quarantine and short lockdowns as required, and widespread vaccination is critical to our society coping with the changes.
Harm caused by Media & Lockdowns
Unfortunately, negative and mixed messages by the media are contributing to fear and COVID anxiety in the community! People are presenting to their doctors with high levels of stress, mental health issues such as anxiety, depression, Post Traumatic Stress Disorder (PTSD), loneliness, boredom, harmful alcohol and drug use, self-harm, suicidal thoughts, burnout, and fatigue.
Repeated and extended lockdowns have escalated COVID anxiety and stress due to isolation, loss of employment, business disruption and/or collapse, uncertainty, and staying home more than usual. Residents living in Victoria and NSW have been most impacted in recent times due to extended long lockdowns. People are feeling frustrated as the lockdowns have disrupted their usual activities e.g. socializing especially for the young people. Children home schooling is a real challenge for many young families. Family violence has escalated. People are feeling fatigue and burnout, and this is contributing or exacerbating chronic mental health illnesses. All age groups can be impacted.
Women impacted by Lockdowns
Women are more impacted than men during lockdowns. Homeschooling with extended lockdowns has placed enormous stress on families and we are hearing of children and parents experiencing daily meltdowns.
Recent research reveals the triple stress load on women who are juggling
- Paid work outside their home
- Taking care of their family especially home schooling, and
- Carrying the “mental labour of worrying” to manage the emotions of their children and/or their partner, to keep the peace & facilitate order in the family.
Victorian women during lockdowns are more likely than men to feel
- nervous (40% compared with 30% men),
- lonely (28% compared with 16% men) and
- “that everything is an effort” (30% compared with 22% men).
Doctors and Healthcare workers
Doctors and healthcare workers are also impacted by COVID stress. A recent Australian Nationwide survey between 27th August till 23rd October 2020, of 7,846 hospital workers [nurses (39.4%), doctors (31.1%), allied health staff (16.7%), other (6.7%)] found stress levels are high. The study found healthcare workers described their feelings of moral distress related to resource scarcity (58.3%), issues with wearing PPE (31.7%) limiting their ability to care for patients, exclusion of family in hospitals going against their values (60.2%), and fear of letting co-workers down if they were infected (55.0%).
The ongoing stress has led to increased risk of anxiety, depression, PTSD and burnout in hospital workers, and unfortunately the situation is likely to get worse with lockdown restrictions lifting soon as we start to see rising COVID infection cases in Australia.
Smoking and alcohol response to stress
COVID restrictions and periods of lockdowns have led to increased smoking rates, alcohol intake and alcohol related harm such as family violence for some people as a response to stress. This is likely associated with the elevated anxiety and depression. For some people, alcohol consumption has increased during the COVID-19 pandemic, and for others it has reduced. As doctors we should be screening patients for alcohol misuse. It is also important we educate our patients about the harms of smoking, as smoking itself increases the risk of COVID morbidity and can exacerbate mood problems directly too. Mood disorders and depression can also contribute to increase alcohol intake which can cause additional short-term and long-term health related alcohol problems, including aggravation of mental health disorders.
Working from home during lockdown
Working from home, long hours sitting in front of the computer all day can lead to increased risk of musculoskeletal problems particularly the neck, shoulder, back pain; muscle and joint pains, eye strain, headaches, fatigue; boredom from less contact with work colleagues, depression, stress, reduced productivity; restricted lung capacity and breathing; digestive issues e.g. constipation, and weight gain due to reduced activity.
Good advice to give our patients is to be aware of their posture during work. A standup desk may help, having regular breaks every ½ hour by walking around their backyard or locally, stretch, and exercise longer especially with the extra time from not driving to work. Avoid rest times on the internet.
Stress impacts the immune system
Chronic stress may contribute to increased risk of infections and can negatively impact the immune system by suppressing both cellular and humoral measures.
What advise can we give to our patients to cope?
It is important to stay mentally and physically healthy to help develop resilience with the changes required over time by maintaining a healthy lifestyle to ensure the body and immune system are strong to help fight infections – it is likely we will all catch COVID.
A healthy lifestyle gives the body the best chance to recover from an infection. Switch off or limit media exposure and googling, and learn the facts by sticking to official Health or Government sites e.g. daily HealthAlerts by the Dept of Health healthalerts@dhhs.vic.gov.au. Keep things in perspective and reassure the situation is likely to improve with widespread vaccination and public health measures, like in Europe.
Refer to Psychologist and Psychiatrist when required
Counselling, CBT, mindfulness and stress management strategies are helpful for dealing with mood disorders. Mindfulness-based stress reduction (MBSR) and mindfulness CBT (MBCBT) help to alleviate symptoms of mental health problems e.g. depression, anxiety disorder, insomnia, and are useful as adjuncts for management of chronic diseases e.g. cancer, CVD, and chronic pain. They are also important strategies for prevention of mood related problems in healthy adults and children.
Research suggests MBSR improves quality of life, sleep, moods, feelings of relaxation, reduces fight and flight response, and may help reduce pain levels.
The following links are useful resources to provide our patients:
Headspace: https://www.headspace.com/meditation/stress
Beyond Blue:https://www.beyondblue.org.au/get-support/staying-well/relaxation-exercises
Australian Pain Management Association:
- https://www.painmanagement.org.au/2014-09-11-13-35-53/2014-09-11-13-36-47/261-how-to-relaxation,-meditation-and-deep-breathing.html
- https://www.spine-health.com/conditions/chronic-pain/11-chronic-pain-control-techniques
Adapting to the changes - Acceptance
A good place to start is Acceptance of the Pandemic and that it will be with us for some time. As soon as we accept, we start to adapt. If we are to adapt, it is also important to reframe our thoughts by focusing on the positive aspects of lockdowns and Public Health measures such as masks. Masks for example help us to feel more confident in public crowded areas such as shopping centres where airborne transmission of COVID virus can be high and physical distancing is difficult. Public health measures such as hand hygiene, physical distancing, and wearing suitable masks, including eye protection, are important strategies to help prevent viral spread. Avoiding crowded and closed environments may help reduce the spread of viruses that cause respiratory illnesses.
Elderly coping better over COVID
A US study found elderly cope better in lockdown and report better mental health and wellbeing due to being better at adapting & accepting adverse situations:
- By drawing on previous life experience & struggles (e.g. post-war, famine and migration)
- Have learnt to adapt, & use survival skills e.g. growing & spending more time in their vegetable garden
- Their focus is more on what is important in life
- Over lockdown elderly had more contact with their children & grandchildren, usually by phone.
Positive aspects of Lockdown & Public Health measures
Influenza infection rates in Australia has been the lowest with only 462 notifications of laboratory-confirmed influenza, no influenza-related deaths, and no influenza related hospital admissions! Working from home for some people has been satisfying due to less travel time to work and creating more time for self-care such as exercise. With more exercise, people are spending more time in nature.
There are less vehicles on the road over lockdowns, making them quieter, safer, and resulting in less air pollution and cleaner air.
Blue/green nature buffers stress
A recent study found that people having access to nature such as beaches, parks, and urban forests over lockdowns, experience more health benefits. The main points highlighted in the study were that nature contact ‘buffers’ the negative effect of lockdown on mental health, helped people cope better with lockdown measures, and was associated with more positive emotions.
Focus on healthy lifestyle
COVID lockdowns are a great opportunity for the community to focus on improving their health and well-being through lifestyle and positive behavioural changes to help support their immune system. Daily exercise, adequate sun exposure, vitamin D in high risk patients, good nutrition and eating well to address nutritional status, and positive behavioral and lifestyle approaches are essential to support the immune system. Smoking avoidance; breathing clean air; addressing obesity and chronic diseases, such as diabetes all play an important role in supporting the immune system.
Exercise and the immune benefits
Apart from general health benefits such as CVD and diabetes control, daily moderate exercise is important for supporting the immune system, for increasing vitamin D levels from natural sun exposure and helps to manage stress and anxiety, and improves sleep. About 30-40 minutes daily of natural sun exposure helps the circadian rhythm to restore good sleeping patterns. Yoga can be practiced at home using free online sites and may assist with depression and anxiety.
Mediterranean diet
A healthy, balanced diet high in vegetables, fruit, nuts, seeds, legumes, and meats [preferably fish] is vital for supporting the immune system, preventing nutritional deficiencies and helping reduce the incidence of respiratory infections. The gold standard Mediterranean diet has been shown to improve and support the immune system and reduce inflammation. The ‘Western diet’ high in saturated fats, is associated with immune dysfunction and higher risk of inflammation.
Studies have found high plant based and/or pescatarian diets are associated with lower risk and severity of COVID-19 infection, and lower COVID mortality. The Mediterranean diet is widely studied and important for prevention and management of chronic diseases. Fast foods are associated with lowered immunity, high risk of infections and depression. Whilst caffeine in low doses can help depression, high doses can cause anxiety particularly in sensitive people. Chamomile tea may be calmative.
Prevalence of Vitamin D deficiency in Australia
The Australian Bureau of Statistics National Health Surveys demonstrate that about 23% of Australian adults have vitamin D deficiency. Vitamin D levels vary considerably by season, with the highest prevalence of vitamin D deficiency in winter, especially in the lower latitudes of Australia, such as Melbourne.
According to Vitamin D and health in adults in Australia and New Zealand, vulnerable groups with greatest risk of vitamin D deficiency include the housebound, community-dwelling older and/or disabled people, those in residential care, dark-skinned people (particularly those modestly dressed), and other people who regularly avoid sun exposure or work indoors. Only 5–10% of vitamin D requirements are sourced from dietary sources. Sunshine exposure is the main source of vitamin D production by the body.
Clinical Benefits of Vitamin D
If deficient in vitamin D, supplementation may be required to help prevent respiratory tract infections. Vitamin D is important for bone and muscle health and regulates calcium levels in the blood, and in the prevention of rickets, osteoporosis and osteomalacia. Vitamin D also plays an important role in regulating the body’s immune response to respiratory viruses and has antiviral effects. Vitamin D is also important for pulmonary function in young adults, inhibits pulmonary inflammatory responses, and modulates innate defence responses to respiratory viral pathogens.
Sun exposure for vitamin D deficiency
A recent article published in the American Journal of Infection Control found a highly significant, positive correlation between lower death rates and a country’s proximity to the equator and COVID-19 mortality. Mortality may correlate with northerly (and possibly southerly) latitude suggesting a possible link with ultraviolet and vitamin D according to another article published in BMJ Nutrition, Prevention and Health. More research is required to verify this observation.
Vitamin D supplements and risk of acute respiratory infections
A meta-analysis found vitamin D (D3 or D2) supplementation was safe and may reduce the risk of acute respiratory tract infections (ARTIs), especially among those who received daily or weekly vitamin D supplements in individuals with severe deficiency (25(OH)D concentration < 25 nmol/L) at baseline. However, there was much heterogeneity and confounders in the study and more research is required.
Vitamin D supplements and risk of COVID-19 infection
Research suggests Vitamin D status may play a role in the prevention, risk and mortality associated with COVID-19 but a recent Mendelian randomization study and Cochrane review 2021 found insufficient evidence to determine the benefits and harms of vitamin D supplementation as a treatment of COVID‐19. It is encouraging that there are a number of clinical trials underway. A recent meta-analysis yet to be rigorously peer reviewed demonstrates benefits. The CORONAVIT trial aims to assess vitamin D risk and severity of COVID-19 and other ARTIs. In the meantime, safe and appropriate sun exposure is advised and take Vitamin D supplements if deficient in high-risk individuals.
Insomnia impacts well-being
1/10 of Australian adults suffer sleep problems. Insomnia affects learning, memory, decision making and moods. Chronic insomnia is associated with feelings of exhaustion and fatigue, and can impair immune responses to infections, especially shorter duration of sleep. Tips for insomnia include
- Behavioural & sleep hygiene advice
- Exercise
- Natural sun exposure to help the circadian rhythm
- Relaxation / meditation
- Bath / soft lighting / downtime before bed as it triggers the pineal gland to release melatonin
- Avoid stimulants e.g. caffeine after 2pm
- Melatonin 2mg SR supplements are now available over the counter in 55-year-old and over.
Nutritional supplements
It is more important to obtain our nutrients for supporting our immune system through diet, but let’s explore some of the evidence available for single nutrients for URTI viruses. Research for their use in COVID is lacking. More research is required in this field. A 2013 Cochrane review found regular supplementation with oral vitamin C was not helpful, although some trials demonstrated that vitamin C reduced cold duration. A meta-analysis demonstrated oral zinc supplementation may shorten the duration of symptoms of the common cold in adults. The use of zinc gluconate lozenges by children may shorten cold duration by an average of two days and reduce the risk of mean number of cold events per year. Another meta-analysis found short term use of zinc acetate lozenges commenced within 24 hours at onset of an URTI, resulted in shortening the duration of symptoms.
Greeks have for thousands of years appreciated the value of garlic in food and for ritual purposes. But what about garlic supplements? A Cochrane review identified a small randomised placebo control trial that demonstrated garlic supplement for 12 weeks resulted in less occurrences of common cold, although more studies are needed to validate this finding. The addition of garlic to the diet is safer and tastier!
Probiotics are found naturally in food sources such as yoghurt. A 2015 Cochrane review demonstrated oral probiotics, Lactobacillus and Bifidobacterium was helpful in reducing the episodes and the duration of acute URTI, with a reduction in needing antibiotics and school absences in children. Another meta-analysis identified that most studies are of low quality but demonstrated probiotics significantly reduced the number of days of illness per person and the days absent from day-care, school, or work.
Key public health messages
Improving lifestyle such as reducing stress, daily exercise especially in open natural space, increasing appropriate natural sun exposure for vitamin D, and/or taking vitamin D supplements in high-risk individuals, and a healthy Mediterranean diet are major key public health messages that may help individuals to support their immune system and deal with viral infections better, whether that may be for COVID-19, influenza, or other common respiratory viruses. Creating a healthy lifestyle program can help us deal with the COVID stress. Current public health measures set by health authorities are particularly effective in reducing risk of COVID infection

